After Elodie Trouche tested positive for the BRCA gene in 2015, she decided to pursue a preventative double mastectomy — but on her terms.

Trouche, 45, a French native now living in Nyack, opted for the test after her sister’s breast cancer diagnosis in 2015.
The results were the beginning of Trouche’s two-year search for a team of surgeons who could perform a nipple-sparing mastectomy, which removes breast tissue while saving the existing nipple and areola, and her search led her to Long Island Jewish Medical Center in New Hyde Park.
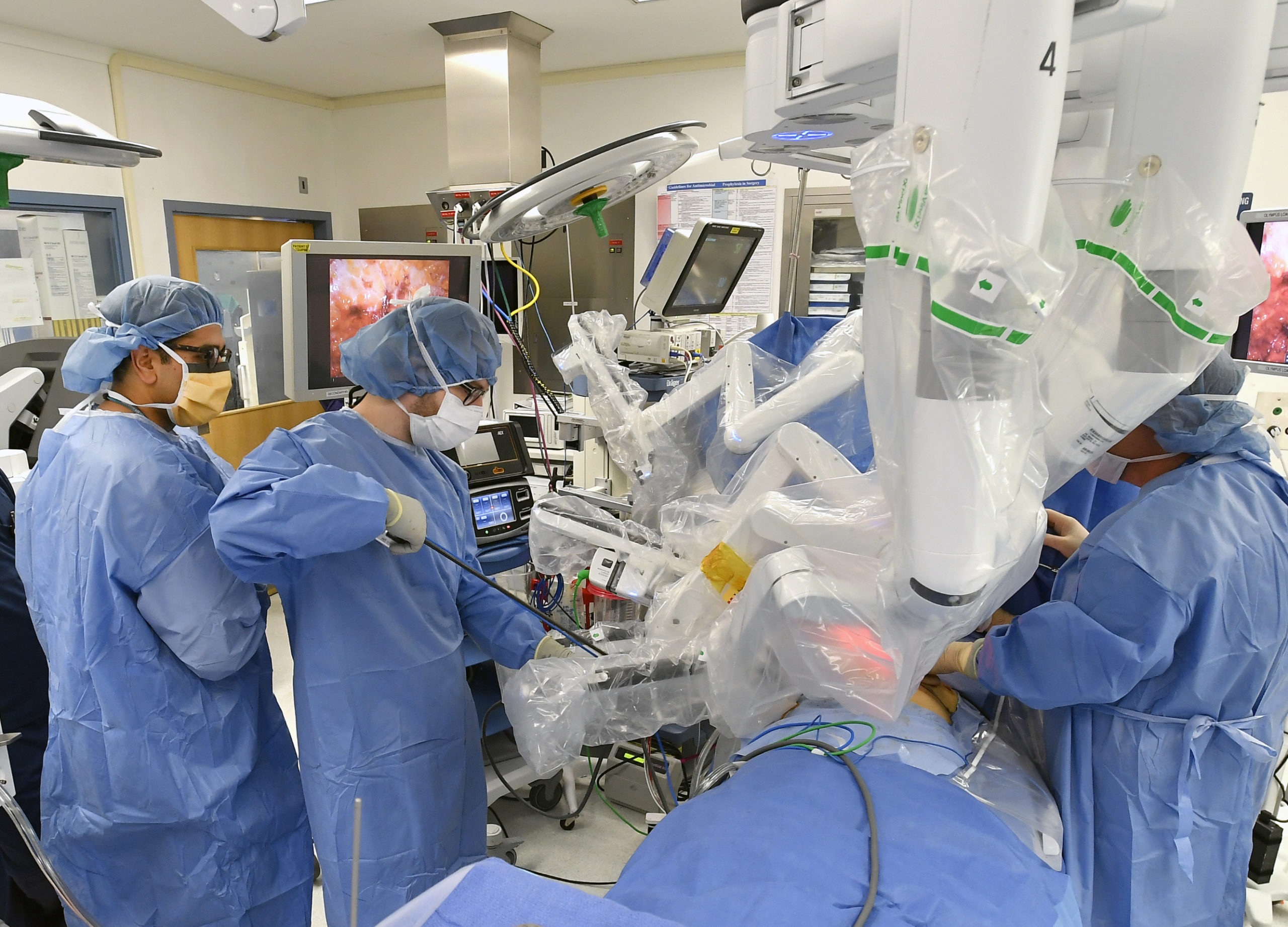
Trouche was the first patient in the United States to undergo a robotic nipple-sparing mastectomy and breast reconstruction surgery on March 4 and spoke of her experiences alongside her surgeons, Dr. Alan Kadison and Dr. Neil Tanna at a news conference on March 6.
Trouche said despite her test results, she “refused to be mutilated.”
“I knew I had some time because I was having surgery as a preventive measure. I wasn’t sick,” Trouche said during the news conference. “I knew about robotic surgery and made up my mind that this was the best way for me. Once I found my team here at LIJ, I never looked back. I have found this entire experience to be very empowering. By educating myself and saying ‘no’ to what I didn’t want, I had the exact type of surgery that I was hoping for.”
According to the National Cancer Institute, about 12 percent of women in the general population will develop breast cancer sometime during their lives.
By contrast, a recent study by the institute estimated about 72 percent of women with a BRCA1 mutation and about 69 percent of women with a BRCA2 mutation will develop breast cancer by age 80.
Tanna said traditionally conventional forms of nipple-sparing mastectomies involved a long incision on the breast itself.
“By doing the surgery robotically, incisions and scars are placed away from the breast, sitting instead on the chest wall near the armpit,” Tanna said. “This surgery was performed as an investigational study following strict Institutional Review Board protocols. We hope to be continuing this study with other women who are interested in considering this alternative to traditional surgery.”
Kadison said he has seen advantages to using the Da Vinci technology for nipple-sparing mastectomies because it gives patients a shorter hospital stay, less post-surgery pain and an easier recuperation period.
“So many women will be affected by breast cancer or the threat of it because of the BRCA gene,” Trouche said. “Through education and empowerment, we can learn about new technology that will help us get through this together.”