Physicians from North Shore University Hospital, the Feinstein Institute for Medical Research and Lenox Hill Hospital in Manhattan, are participating in a clinical research study testing whether intraoperative radiotherapy is more effective at preventing tumor regrowth than standard therapy for one of the most aggressive forms of brain cancer – glioblastoma multiforme (GBM).
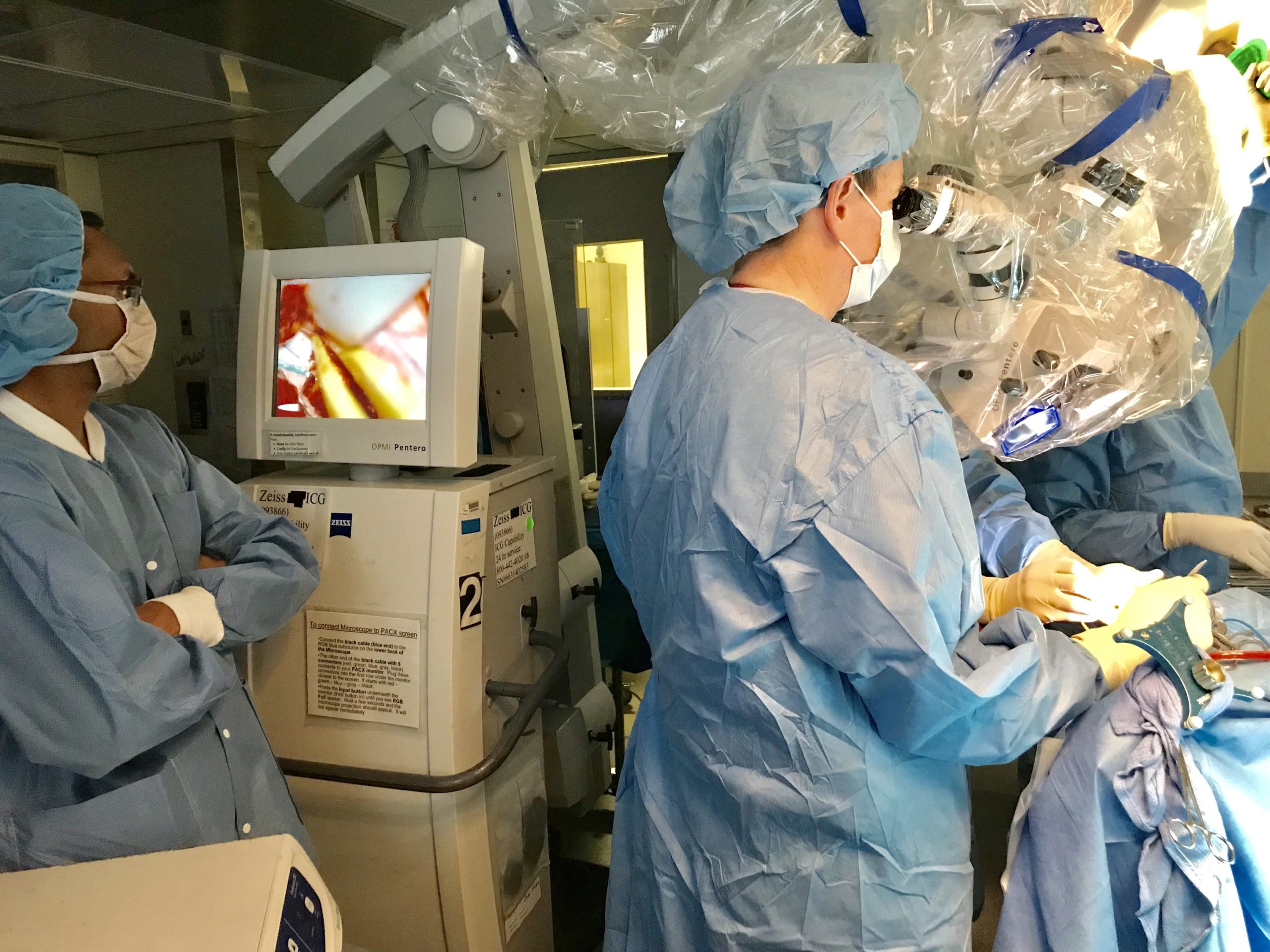
A 53-year-old man from Queens was the first GBM patient in New York State to receive IORT in the study during a procedure performed by neurosurgeons Dr. Michael Schulder, MD and Dr. David Weintraub, along with radiation oncologist Dr. Anuj Goenka at North Shore University Hospital. Schulder, director of Northwell Health’s Brain Tumor Center at the Institute for Neurology and Neurosurgery, Dr. John Boockvar, director of Lenox Hill’s Brain Tumor Center, and Goenka, co-director of Northwell Health’s Center for Stereotactic Radiosurgery, are working together as investigators of the study entitled, “A Multicenter, Randomized Phase III Study on Intraoperative Radiotherapy in Newly Diagnosed Glioblastoma Multiforme.” Also known as the INTRAGO study, it is being sponsored by the University of Heidelberg in Germany.
“We are constantly looking for new treatments in the fight against GBM,” said Schulder. “Immediately after tumor resection, IORT delivers a concentrated, high dose of radiation therapy to the tumor bed and is performed in the operating room, in a single treatment session. The precisely targeted radiation helps destroy any microscopic tumor cells that may be left behind and also allows for the preservation of healthy surrounding tissue.”
Participants in the research study will be randomized into two groups: one group will receive standard of care treatment while the other cohort will receive standard of care and intraoperative radiotherapy. Standard of care involves a traditional tumor resection, followed by six weeks of external beam radiation therapy concurrently while receiving the chemotherapy drug, Temozolomide.
The other group will receive standard of care and intraoperative radiotherapy, in which the neurosurgeon first removes the brain tumor in the same way that is traditionally done with a craniotomy. Following the tumor resection, the radiation oncologist inserts a mobile X-ray device – the IntrabeamÒ System – into the skull, allowing for high doses of radiation to be delivered directly to the tumor site. The radiation process can take approximately 20-60 minutes. After radiotherapy is completed, the device is removed and the surgeon closes the site. Patients have recovered from this procedure just as well as after conventional brain tumor removal. Approximately five weeks after surgery, the normal standard of care of chemotherapy and radiation is also given.
“We hope this will help build on our current treatment arsenal for this disease,” said Goenka. “The initial data that this study is based on is very promising.”